If your mood drops sharply before your period, you’re not imagining it. Pre-period depression is a real, recognized pattern, and for some people, it’s severe enough to have a clinical name.
When symptoms go beyond ordinary moodiness and significantly disrupt daily life, it may be premenstrual dysphoric disorder, or PMDD. For women already navigating mood difficulties, outpatient mental health treatment can offer structured, individualized support for understanding and addressing cyclical patterns like these.
Quick Takeaways
- Pre-period depression is tied to how the brain responds to hormonal shifts in the weeks before your period.
- When symptoms are severe and predictably cyclical, the cause may be PMDD, a diagnosable mood disorder distinct from PMS.
- Serotonin sensitivity appears to play a central role.
- PMDD frequently co-occurs with depression, anxiety, and trauma histories.
- Effective options exist, from therapy and medication to structured outpatient programs.
What’s Happening in Your Brain Before Your Period
Your brain responds to hormonal changes, and some brains respond more intensely than others.
During the luteal phase, which runs from ovulation to the start of your period, estrogen and progesterone rise and then fall sharply. For most people, this happens without significant emotional disruption. For others, the brain’s serotonin system appears to be more sensitive to these fluctuations. [1]
Serotonin regulates mood, sleep, appetite, and emotional stability. In people with PMDD, research suggests the brain’s serotonin system becomes less efficient during the premenstrual phase, producing symptoms that can look a lot like clinical depression. [2]
The key difference for individuals with PMDD is that the symptoms lift shortly after the period begins. That predictable, cyclical pattern is what sets the condition apart from other mood disorders.
What Is PMDD, and How Is It Different from PMS
PMS is common. Most people experience some physical or emotional changes before their period.
PMDD, on the other hand, is more severe and more disruptive than PMS. According to the Cleveland Clinic, PMDD causes severe mood-related symptoms, including intense irritability, anxiety, and depression, on top of physical symptoms like bloating or cramping. [3] The pattern must interfere significantly with daily life, relationships, or work.
It’s important to note that PMDD is a distinct clinical condition—it is not the same as PMS.
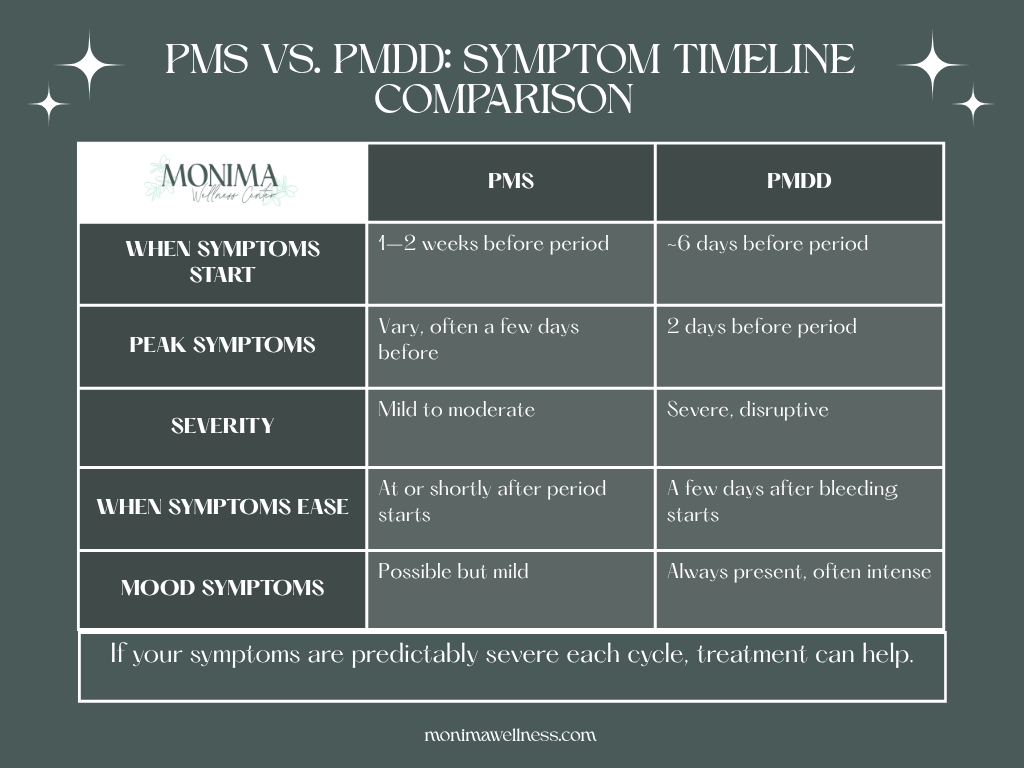
What Are the Symptoms of PMDD
PMDD symptoms vary from person to person, but mood-related symptoms are always part of the picture. They typically begin around six days before menstruation and are most severe in the two days just before bleeding starts. [1]
Of all PMDD symptoms, anger and irritability tend to be the most distressing and often appear before the others. [1]
Common symptoms include:
- Persistent sadness, hopelessness, or feeling on the verge of tears
- Intense irritability or anger that feels disproportionate
- Anxiety or a pervasive sense of being overwhelmed
- Difficulty concentrating or following through on tasks
- Changes in sleep, appetite, or energy
- Loss of interest in relationships or activities
- In more severe cases, thoughts of hopelessness or worthlessness
Most of the time, these symptoms begin to ease within a few days of the period starting.
Who Is Most Likely to Experience Premenstrual Depression
Some people are more sensitive to luteal-phase hormonal shifts than others, and research points to a few consistent risk factors.
PMDD is more common in people with a personal or family history of depression, anxiety, or seasonal affective disorder. [1] Thyroid dysfunction, high chronic stress, and disrupted sleep can also increase susceptibility. A history of trauma is also a recognized risk factor, with traumatic events and pre-existing anxiety disorders both associated with PMDD development. [1]
PMDD can affect anyone who menstruates. It’s most often identified in people in their mid-twenties to mid-forties, but it can occur at any point during the reproductive years. [1]
It’s also frequently underdiagnosed. This is because cyclical mood symptoms are often dismissed as personality or stress, rather than as a treatable condition.
How PMDD Is Diagnosed
There’s no lab test for PMDD. Diagnosis is based on symptom tracking.
A diagnosis requires documenting symptoms using a validated tool, such as the Daily Record of Severity of Problems (DRSP), across at least two menstrual cycles to confirm the pattern and timing. [4] That cycle documentation is what makes PMDD diagnosable and distinguishes it from other mood disorders.
A thorough evaluation should also rule out overlapping conditions, such as thyroid disorders, major depressive disorder, or generalized anxiety. Treating the wrong condition leads to incomplete results.
If you’re noticing a cyclical pattern in your mood that’s impacting your daily life in a meaningful way, it’s worth exploring. At Monima Wellness, our on-site psychiatrist specializes in women’s mental health and reproductive psychiatry, and every client receives hormone testing and comprehensive neuropsych testing as part of their care. Reach out to our team to learn more.
What Helps PMDD Symptoms
PMDD responds to treatment. The right approach depends on symptom severity and what’s co-occurring.
Lifestyle: Regular aerobic exercise throughout the month is among the most well-supported options for reducing PMDD severity. Reducing caffeine, alcohol, salt, and sugar, especially during the luteal phase, can also stabilize mood and energy. [3]
Therapy: Cognitive behavioral therapy (CBT) has demonstrated effectiveness for PMDD. It helps people build coping strategies for the most symptomatic days and recognize thought patterns that amplify distress. [5]
Medication: For moderate to severe PMDD, SSRIs are often a first-line option. They work rapidly in PMDD, often within days, which is distinct from how they function in other depressive disorders and points to a serotonin-specific mechanism. [5] SSRIs can be taken throughout the cycle or only during the luteal phase. Certain hormonal contraceptives, particularly those containing drospirenone, have also shown effectiveness. [4]
When PMDD is severe or co-occurs with depression, anxiety, or trauma, structured outpatient support may be helpful in stabilizing symptoms. Partial Hospitalization (PHP) and Intensive Outpatient Programs (IOP) provide consistent, integrated care while allowing people to maintain work, school, and daily responsibilities.

Find Relief From PMDD
If premenstrual depression is affecting your daily life, you don’t have to navigate it alone. Call us at 858-500-1542 or verify your insurance coverage to find out what options may be covered.





